Eating Disorder Hope is a leader in the online Pro-Recovery Movement. We are passionate about helping those in eating disorder recovery find hope, health, and healing. With the understanding that recovery allows you to fully participate in life and contribute to the world around you in meaningful ways, we are honored to support your journey and give you a platform to share your voice.
How to Evaluate the Medical Support of an Eating Disorder Treatment Program?
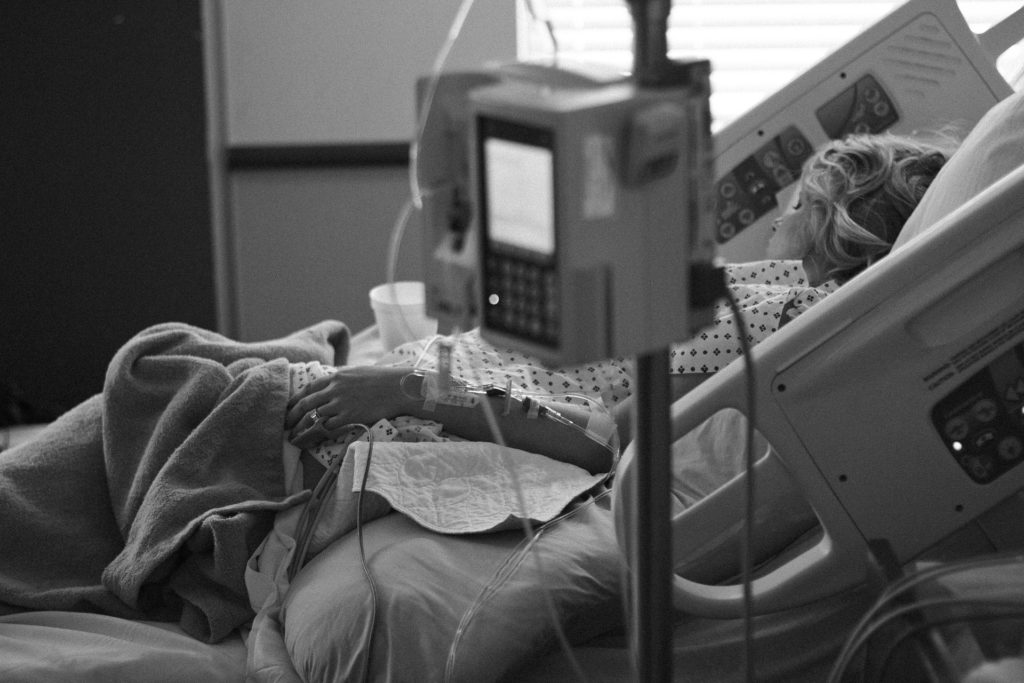
Eating disorders are complex. Marked by severe discrepancies in a person’s eating behaviors, eating disorders have the potential to not only affect a person’s physical and mental health but in some cases, can be life-threatening. However, treatment does exist, and so does hope for recovery. In order to make an informed decision, it is best to evaluate all aspects of a treatment program, including medical support for eating disorders.
Medical aspect of eating disorder treatment
Eating disorders often involve an interconnection between psychology and medicine. Numerous medical complications accompany an eating disorder, including high blood pressure, diabetes, obesity, and heart problems, among many others. Such adverse medical morbidities need to be diagnosed and promptly treated.
Having medical professionals at the facility can be highly important so that they can monitor and evaluate any medical conditions that a patient may have. Often medications are needed to manage conditions and maintain nutrients, and the dosages need to be monitored by a professional. It is essential to ask about the role of medications in treatment and how will they be administered.
Patients with anorexia nervosa benefit largely from psychotherapy and medications should only be used as an adjunctive component. Bulimic patients and those with binge eating disorder, however, benefited significantly from pharmacotherapy.
Even though psychological symptoms may dominate the presentation of this disorder, a medical physician is an integral part of the treatment team and can play a unique role in the diagnosis and treatment of eating disorders. In fact, among adults with eating disorders, almost half were first diagnosed by their primary care physician.
Health services utilization is relatively high in this population. Weight restoration often precedes an eating disorder treatment program and typically takes place in a hospitalized setting. The choice between medical or psychiatric hospitalization is based on resources available, medical condition, and age of the patient.
The patient should remain in the hospital until their physical condition is stable, mental status improves, and a care plan is determined. One study found that those eating disorder patients who remained in the hospital until they had regained adequate weight had a better outcome compared with those who did not.
What constitutes good medical support for eating disorders?
A positive environment: It is essential for the treatment setting to offer a nurturing environment constituting of an experienced staff that is specially trained in treating eating disordered patients. Staff should be understanding, empathetic, and accommodating, and to be able to assist patients transitioning back to normal life.
Individualized treatment: Each patient is influenced by different biological, psychological, and social factors. It is vital to curate individual treatment plans for each patient. Alongside group therapy, individual therapy is necessary in order to address each patient’s underlying issues, which helps them feel validated.
All-encompassing treatment model: In addition to individual and group sessions, it is essential for the treatment center to have a family program as well that constitutes of family therapy. Furthermore, you need to ask what skills and coping strategies are taught to the patient. Is the patient being helped with co-occurring conditions like anxiety, depression, and relationship issues?
 Adequate medical services: Presence of medical professionals and their availability at the facility is an essential element of treatment that needs to be considered during an evaluation. Health problems are often plaguing patients of disordered eating and addressing them is just as important, if not more, as psychological issues are.
Adequate medical services: Presence of medical professionals and their availability at the facility is an essential element of treatment that needs to be considered during an evaluation. Health problems are often plaguing patients of disordered eating and addressing them is just as important, if not more, as psychological issues are.
Psychiatric services: Psychiatrists should be an integral part of the staff to evaluate co-occurring conditions like anxiety, depression, and obsessive-compulsive disorders among several others. The rate of coexisting psychiatric conditions is high with eating disorders, and most often is what is fueling the disorder in the first place.
Looking ahead
When evaluating a treatment program’s medical support for eating disorders, it is important to pay attention to the availability and accessibility of a medical professional on the treatment team, the role of medications and how co-occurring health problems will be addressed throughout treatment.
Most patients benefit from a multidisciplinary approach, often involving specialized psychological treatment, medication management, and medical monitoring. Patients with eating disorders generally should be cared for by a multidisciplinary team consisting of a medical doctor, psychiatrist, therapist, and a dietitian.
References:
1. https://eatingdisordersadvisors.com/how-to-assess-eating-disorder-finds-support-services
2. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3000192/
3. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2912736/
About the Author:
 Sana Ahmed is a journalist and social media savvy content writer with extensive research, print, and on-air interview skills. She has previously worked as a staff writer for a renowned rehabilitation institute, a content writer for a marketing agency, an editor for a business magazine and been an on-air news broadcaster.
Sana Ahmed is a journalist and social media savvy content writer with extensive research, print, and on-air interview skills. She has previously worked as a staff writer for a renowned rehabilitation institute, a content writer for a marketing agency, an editor for a business magazine and been an on-air news broadcaster.
Sana graduated with a Bachelors in Economics and Management from the London School of Economics and began a career of research and writing right after. Her recent work has largely been focused upon mental health and addiction recovery.
The opinions and views of our guest contributors are shared to provide a broad perspective of eating disorders. These are not necessarily the views of Eating Disorder Hope, but an effort to offer a discussion of various issues by different concerned individuals.
We at Eating Disorder Hope understand that eating disorders result from a combination of environmental and genetic factors. If you or a loved one are suffering from an eating disorder, please know that there is hope for you, and seek immediate professional help.
Reviewed & Approved on June 19, 2019, by Jacquelyn Ekern MS, LPC
Published June 19, 2019, on EatingDisorderHope.com

The EatingDisorderHope.com editorial team comprises experienced writers, editors, and medical reviewers specializing in eating disorders, treatment, and mental and behavioral health.


